On Wednesday, April 29, Rabin Martin, as the Secretariat for the Private Sector Roundtable for Global Health Security (PSRT), hosted a 10th call in a series on the latest health impacts of COVID-19. The call featured Dr. Margaret Bourdeaux and Dr. Vanessa Kerry from Harvard Medical School’s Department of Global Health and Social Medicine and Harvard Kennedy School’s Belfer Center for Science and International Affairs, Security and Global Health Project. Drs. Bourdeaux and Kerry offered their perspectives on translating experiences from conflict zones towards building more enduring public health systems – at home and abroad – and the critical importance of global health security.


Drs. Bourdeaux and Kerry both discussed the imperative to build the “global immune system” to prevent exactly the kind of health emergency that the world is now confronting with COVID-19. Reflecting on learnings from conflict zones where health systems are weak, they emphasized the need to invest in 1) well governed, equitable health systems; 2) innovation pipelines to produce countermeasures; and 3) health security governance.
Dr. Bourdeaux highlighted the often-overlooked indirect contributors to death and morbidity following a disaster, noting that humanitarian crises, health emergencies and earthquakes tend to kill more people indirectly. Knock-on impacts – including economic fallout, people driven into poverty, collapse of health systems – are ultimately more destructive than the immediate health toll. She added that the Ebola outbreak in West Africa in 2014-2015 infected 26,000 people and 11,000 of them died, however the crisis led to a $53 billion downturn in the regional economy.
The challenge is communicating these dangers – even though they are obvious in the moment – in a way that prompts timely preventive action in the public health sphere, even as attention shifts to economic recovery. This is true currently with the COVID-19 response: “The temptation in the U.S. is to bring a bazooka to the economic crisis, but a water pistol to the health crisis.”
Dr. Bourdeaux added that in many countries, there has been a “hollowing out” of health systems – including the primary care system in the U.S. Where health systems are weak, they struggle more with epidemics. Dr. Kerry added that the most fragile systems will be the hardest hit and least able to care for their populations.
And while many think of health systems as just labs, testing agents and infrastructure, Dr. Bourdeaux commented that the relationship between individuals and their health providers to solve routine problems is the underpinning of a robust health system. Likewise, she emphasized that an epidemic is worse when people don’t trust their health system: “Trust is the biggest intervention in promoting health security.”
Dr. Kerry added that health security is national security and that a failure to invest in health meaningfully will leave us all vulnerable: “We are only as strong as our weakest neighbor.”
She urged a shift in thinking about health – moving away from health as a charitable or scientific enterprise to viewing health as a prerequisite for security. “We need to get more serious about building health systems around the world to detect and contain emerging threats because we are all depending on other countries to keep us safe.”
In terms of the private sector’s role, both urged that companies speak up about the need to invest in primary health care and health governance – and also invest in policy conversations and forums to bring security, financial and health policymakers to the same table.
Likewise, Dr. Kerry noted that the willingness of businesses to invest in the health of their own workforce and communities will go a long way toward protecting populations, improving community wellness and reducing vulnerabilities. If a company’s workforce gets sick, it’s harder to do business: “We need to think more holistically about a well-being agenda which would help businesses become more sustainable and lead to a steadier state of growth and prosperity.”
Pandemic Spread
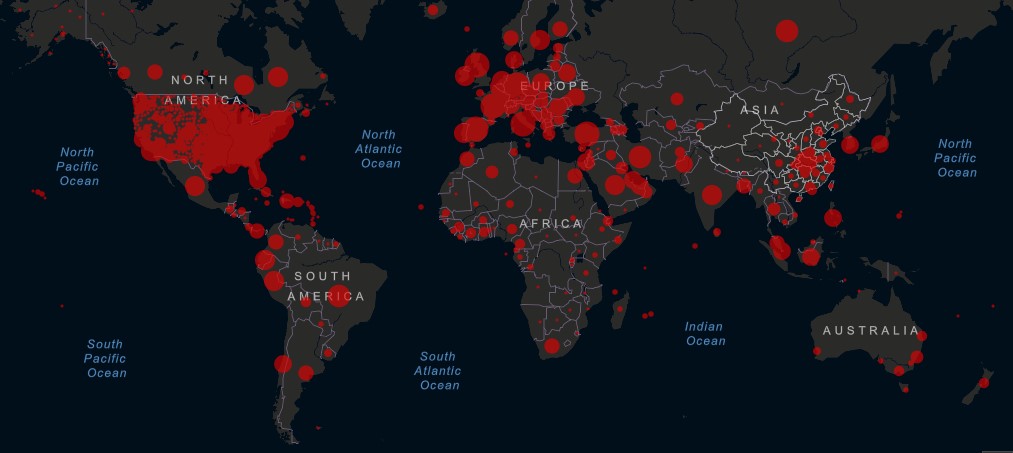
This week, the global community passed the tragic milestone of reporting 3 million cases of COVID-19 worldwide. Confirmed cases in the U.S. now total more than 1 million, but experts warn that the true number is undoubtedly significantly higher. The U.S.’s poor testing strategy has hamstrung the country from the beginning of its response, and limited access to tests continue to produce unreliable estimates for total cases. The focus on measuring deaths by positive tests alone underestimates the number of individuals dying of usually treatable conditions, like heart attacks, because they are unable to access care in an overburdened health system.
Worldwide, as of Thursday, April 30 at 1:30 pm ET, the Center for Systems Science and Engineering at Johns Hopkins University reported 3,231,701 confirmed cases and 230,615 deaths attributed to COVID-19.
There is no longer any question that the U.S. is confronting the worst COVID-19 epidemic across the globe. The question now is how the U.S. will move forward in its response. On Monday, April 27, the Trump administration unveiled a “Blueprint” for testing and rapid response programs to reopen the country. Key among the Blueprint’s promises is a dramatic expansion of U.S. testing capabilities to run 2 million tests per week. Experts warn that the need for testing varies by state and, even with expansion, many states are significantly below these testing targets. Some experts caution these targets are too low to provide the kind of surveillance data needed to monitor the epidemic and prevent a resurgence of infections. Government officials have expressed further concern that these targets are not attainable given current shortages and under resourcing.
“There is absolutely no way on Earth, on this planet or any other planet, that we can do 20 million tests a day, or even five million tests a day.”
Admiral Brett Giroir, U.S. Assistant Secretary of Health
The Blueprint also relies heavily on antibody testing to identify those who have already had the virus and are presumably safe to return to work. This recommendation puts the onus on states independently to verify the validity of antibody tests not yet authorized by the FDA, a valid concern given that a review of 14 available antibody tests showed that only three produced reliable results. Furthermore the WHO warned against such reliance on antibody testing saying, “At this point in the pandemic, there is not enough evidence about the effectiveness of antibody-mediate.
Industry Developments
“[The remdesivir trial] is a very important proof of concept. Because what it has proven is that a drug can block this virus.”
Anthony Fauci, Director, National Institute of Allergy and Infectious Disease (NIAID)
“Remdesivir isn’t a home run but looks active and can be part of a toolbox of drugs and diagnostics that substantially lower our risk heading into the fall.”
Scott Gottlieb, former commissioner, FDA
Countering news late last week that Gilead’s experimental antiviral medication remdesivir showed no positive impact in clinic trials in China, the company announced on Wednesday, April 29, that topline results from a trial run by NIAID show that COVID-19 patients “who received remdesivir recovered faster than similar patients who received placebo.”Study data have not been released, leading some to question what a full analysis of the data will show. Still, Dr. Facui is optimistic about the drug’s potential. Comparing the COVID-19 crisis to the beginning of the AIDS crisis, he said, “Similar to AZT, [remdesivir]’s the first baby step towards what hopefully will be a number of better drugs that will come in and be able to treat people with COVID-19.” The U.S. Federal Drug Administration is expected to grant remdesivir emergency use authorization later this week.
-
After launching its new antibody test on Wednesday, April 15, Abbott Laboratories received emergency use authorization from the FDA on Sunday, April 26 and CE Mark for the European Economic Area. Abbott expects to ship 20 million tests in June.
-
Following unpromising data from early trials, Sanofi and Regeneron announced on Monday, April 27, they will be scaling back enrollment in Phase 3 trial of Kevzara, an arthritis medicine that had shown promise as a treatment for COVID-19.
-
On Tuesday, April 28, Novartis announced plans for a Phase 3 clinical trial to evaluate use of canakinumab in patients with COVID-19-induced pneumonia. Canakinumab, an interleukin blocker, is theorized to suppress cytokine storms, a dangerous immune-system overresponse.
In a week of mixed news regarding once-promising therapeutics, CEPI head Richard Hatchett expressed optimism that corporate collaborations could accelerate the already bright timeline of delivering vaccines in 12 to 18 months. Drawing attention to the full spectrum of activities required to develop and mass produce a vaccine, Sanofi CEO Paul Hudson offered a tempered response. Hudson expressed concern as to Europe’s capacity to manufacture a vaccine when a proven candidate becomes available. Sanofi has pushed the European Commission for a coordinated response similar to that led by the Biomedical Advanced Research and Development Authority in the U.S.
“There is less concern about finding a successful vaccine than there is about making the volumes needed.”
Paul Hudson, CEO, Sanofi
“A coronavirus vaccine won’t stop the pandemic without all countries having access to it.”
Seth Berkley, CEO, Gavi
In Memoriam

On Sunday, April 27, Dr. Lorna M. Breen died by suicide at her family’s home in Virginia. Dr. Breen was the Medical Director of the emergency department at New York-Presbyterian Allen Hospital in Manhattan and worked to save the lives of patients infected with COVID-19 – and had been infected as well. To Dr. Breen and all emergency workers, we thank you for your dedication and sacrifice. “Make sure she’s praised as a hero, because she was. She’s a casualty just as much as anyone else who has died,” said Dr. Breen’s father.
If you or someone you know is contemplating suicide, call the National Suicide Prevention Lifeline at 1-800-273-8255. For hotlines in other countries, click here
From the Experts
“[German states’ loosening of social distancing measures] worries me… they appear to be very bold, maybe too bold… Let us not squander what we have achieved and risk a setback.”
Angela Merkel, Chancellor, Germany
Thursday, April 23
“This emergency has distracted a lot of critical work in many, many areas. Fewer people able to show up for routine immunization or supply chains for immunization not working well, that’s hundreds of thousands of deaths right there. If we can’t keep getting malaria treatments out effectively, that’s a huge rebound in malaria.”
Bill Gates, Co-Founder, Bill & Melinda Gates Foundation
Sunday, April 26
“National unity is the foundation for global solidarity. Solidarity, solidarity, solidarity – that’s what we will say every single day. If we’re not united the virus will exploit the gaps between us and create havoc. Lives will be lost. We can only defeat this virus through unity at the national level and solidarity at the global level.”
Tedros Adhanom Ghebreyesus, Director-General, WHO
Monday, April 27
“The blueprint [to expand testing in the US] lays out the roles and responsibilities to enhance our partnership between the private sector and the public sector, bringing together state and local governments with the federal government to ensure that we can accomplish and achieve our core principles and objectives.”
Deborah Birx, Coronavirus Response Coordinator
Monday, April 27
“It’s inevitable that the coronavirus will return next season…When it does, how we handle it will determine our fate.”
Anthony Fauci, Director, National Institute of Allergy and Infectious Disease
Wednesday, April 29
“If you want to make that 18-month timeframe, one way to do that is put as many horses in the race as you can.”
Peter Hotez, Dean,
National School of Tropical Medicine at Baylor College of Medicine
Thursday, April 30
Additional Resources
Reports from International Governments and Bodies
- WHO COVID-19 Information and Guidance
- WHO Situation Reports, April 27, April 28, April 29
- White House Coronavirus Task Force Press Briefings, April 27
- CDC Coronavirus Resource Page
- COVID-19 Health Systems Response Monitor
- NCD Alliance COVID resources relevant to NCDs
Funding and Policy Trackers
- International Monetary Fund Policy Tracker
- Kaiser Family Foundation Coronavirus Policy Tracker
- U.S. Chamber of Commerce Foundation Corporate Aid Tracker
- Devex Interactive Funding Tracker
Resource Pages and Market Research Literature
- JAMA Resource Center
- The Lancet COVID-19 Resource Centre
- 2019 Novel Coronavirus Research Compendium (NCRC)
- PharmaIntelligence: Coronavirus – What will the Impact Be?
- Health Affairs Resource Center
- STAT Preparedness Tool
- International Association of National Public Health Institutes COVID-19 Resources
- Primary Health Care Performance Initiative Forum
- U.S. Global Leadership Coalition COVID-19 Issue Briefs
- Prevent Epidemics Weekly Science Review
Communications Toolkits
What We’re Reading
When epidemics collide, Editorial Team, The Lancet
Drugmakers race to scale up vaccine capacity, Joe Miller and Hannah Kuchler, Financial Times
Funding the development and manufacturing of COVID-19 vaccines: The need for global collective action, Marco Schäferhoff, Gavin Yamey, and Kaci Kennedy McDade, Brookings Institute
Hundreds of miles from home, nurses fight coronavirus on New York’s front lines, Jenny Gross, The New York Times
Consumer beware: Coronavirus antibody tests are still a work in progress, JoNel Aleccia, Kaiser Health News
A time to save the sick and rescue the planet, Antonio Guterres, The New York Times
What policy makers need to know about COVID-19 protective immunity, Daniel Altmann, Daniel Douek, and Rosemary Boyton, The Lancet
The next pandemic: Rising inequality, Charlie Cooper, Politico
At least 89 vaccines are being developed. It may not matter, Seth Berkley, The New York Times